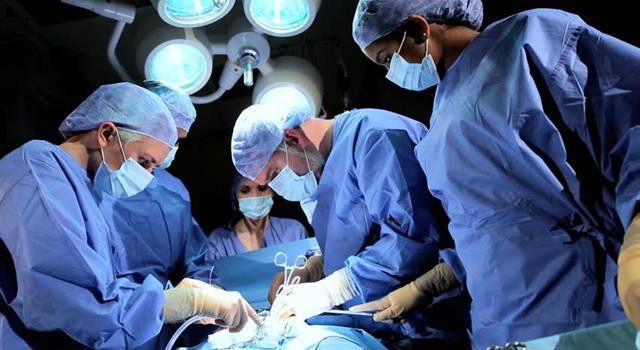
The fact is that the best we can currently hope for is a mechanical heart that lets a patient live long enough to find a donor heart. And when the heart breaks down past the point where medicine or surgery can help, we’re left with far fewer alternatives than someone with a bum knee would face. From prosthetic eyes to artificial hips and knees, there are very few parts of the human body that can’t be swapped out with something that works at least as well as the original, especially given that the OEM part was probably in pretty tough shape in the first place.īut the heart has always been a weak spot in humans, in part because of the fact that it never gets to rest, and in part because all things considered, we modern humans don’t take really good care of it. We will always have patients like Barney Clark who, facing dreaded diseases, take risks that their protectors just don’t understand.The number of artificial prosthetic replacement parts available for the human body is really quite impressive. Few bioethicists truly believe that they can or should singlehandedly circumscribe behaviors. Instances in which patients have pushed the envelope despite warnings include in vitro fertilization, stem cell research, enhancement technologies and entry into stage I clinical trials.īut this dynamic is, ultimately, a good one. In the intervening 25 years, this dynamic has often been repeated: the public rejecting the advice of the very bioethics profession that has sought to protect it. “If, in the process of averting death,” wrote William Safire, then a columnist at the New York Times, “a patient chooses to become a human guinea pig or to marry a bulky machine, the patient has the right to demand that the medical profession let him make that choice.” “Who is so hard of heart as not to be profoundly moved by this historic accomplishment?” asked a Tennessee editorial writer. “I lost a brother to heart disease and suffer from a serious heart problem myself,” one man wrote to Una Loy Clark. Far from seeing Clark as a victim, he was lionized as a hero who had knowingly entered uncharted waters for the benefit of science and future patients. The Clark case, they concluded, was “fundamentally unethical” and “profoundly disquieting.”īut the public's response was quite different. Swazey, who documented several irregularities in the process by which the Utah Institutional Review Board had approved the experiment. The most critical ethical analysis was performed by the team of sociologist Renee C. Annas termed the consent formed signed by Clark “incomplete, internally inconsistent, and confusing.” Caplan, then of the Hastings Center, a New York ethics think tank, believed that animal experiments carried out to date had not been conclusive enough to warrant implantation of the heart in a human. Yet while the University of Utah had tried to heed these new concerns, most bioethicists ultimately criticized what happened. Protecting the rights and bodies of research subjects-and patients-was central to bioethics’ mission. Among the major reasons the field had emerged were a series of research scandals, in which patients had unknowingly been entered into harmful studies. The nascent profession of bioethics paid close attention to Clark from the start. But there were good days, too, such as March 7, 1983, when an interactive Clark celebrated his 39th anniversary with his wife and children. 
It was later revealed that before his death, 112 days after the implantation, Clark had extended periods of confusion and even suicidality. Almost immediately, Clark experienced severe complications, including seizures and a broken heart valve. Although early interest focused on the case’s Frankenstein-like aspects, the public was quickly drawn to the story of an admirable patient, his stoic wife Una Loy and a team of pioneering doctors.īut all was not well. The news that Clark was alert and responsive post-operatively made front-page news around the world. 
Clark’s story reveals both the triumphs and limitations of the bioethics “revolution.” The Clark case was a proving ground for the new field which, in response to a series of crises, had emerged to forge a new paradigm for making medical decisions. When Clark agreed to become the first recipient of a permanent artificial heart 25 years ago, he was exploring new territory not only in medicine but in bioethics. DeVries and his team at the University of Utah removed Clark’s heart and replaced it with an aluminum and polyurethane device connected to a 400-pound air compressor that would accompany Clark for the rest of his life. Barney Clark was a retired dentist who, by late 1982, had developed end-stage heart failure and could barely walk to the bathroom.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
